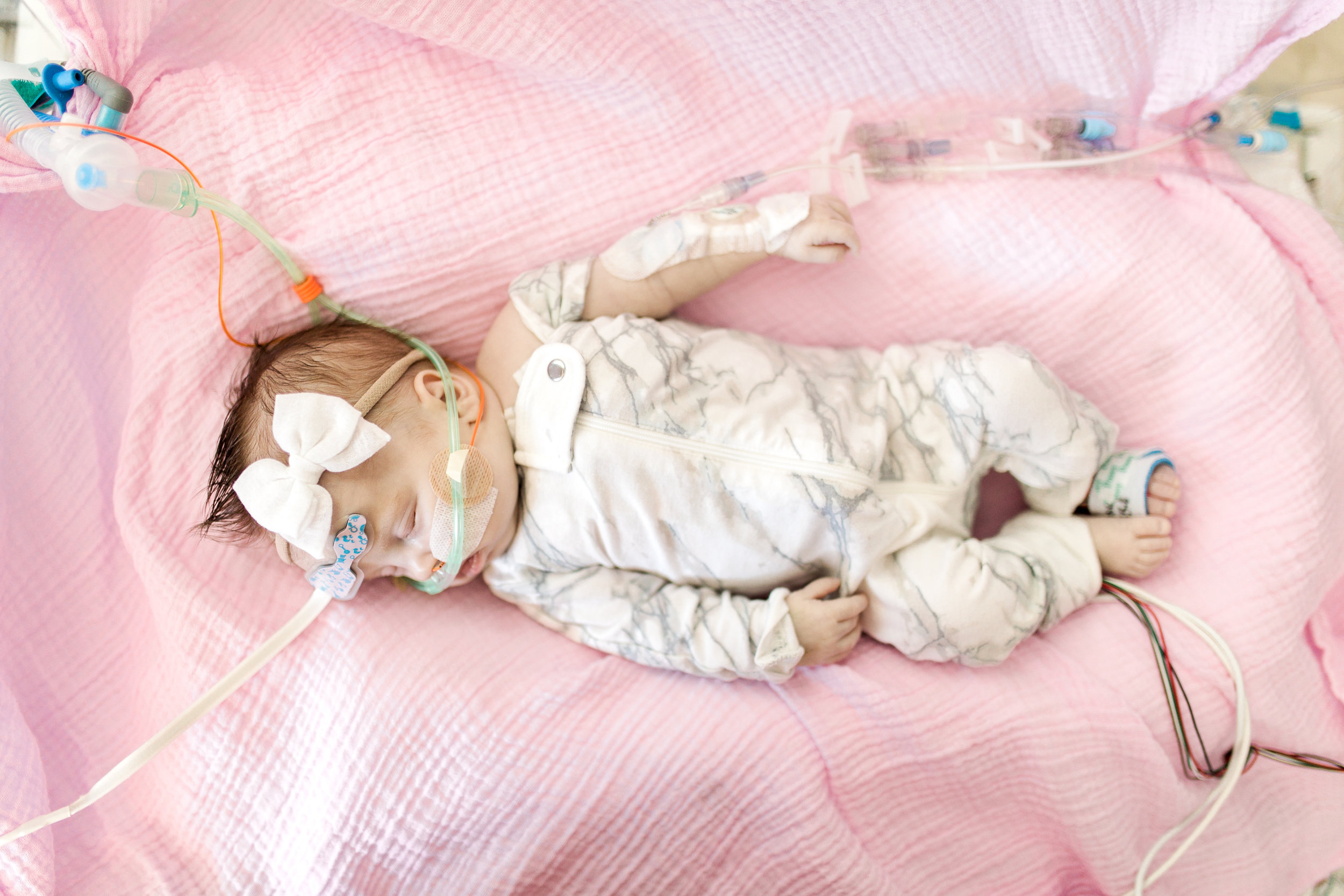
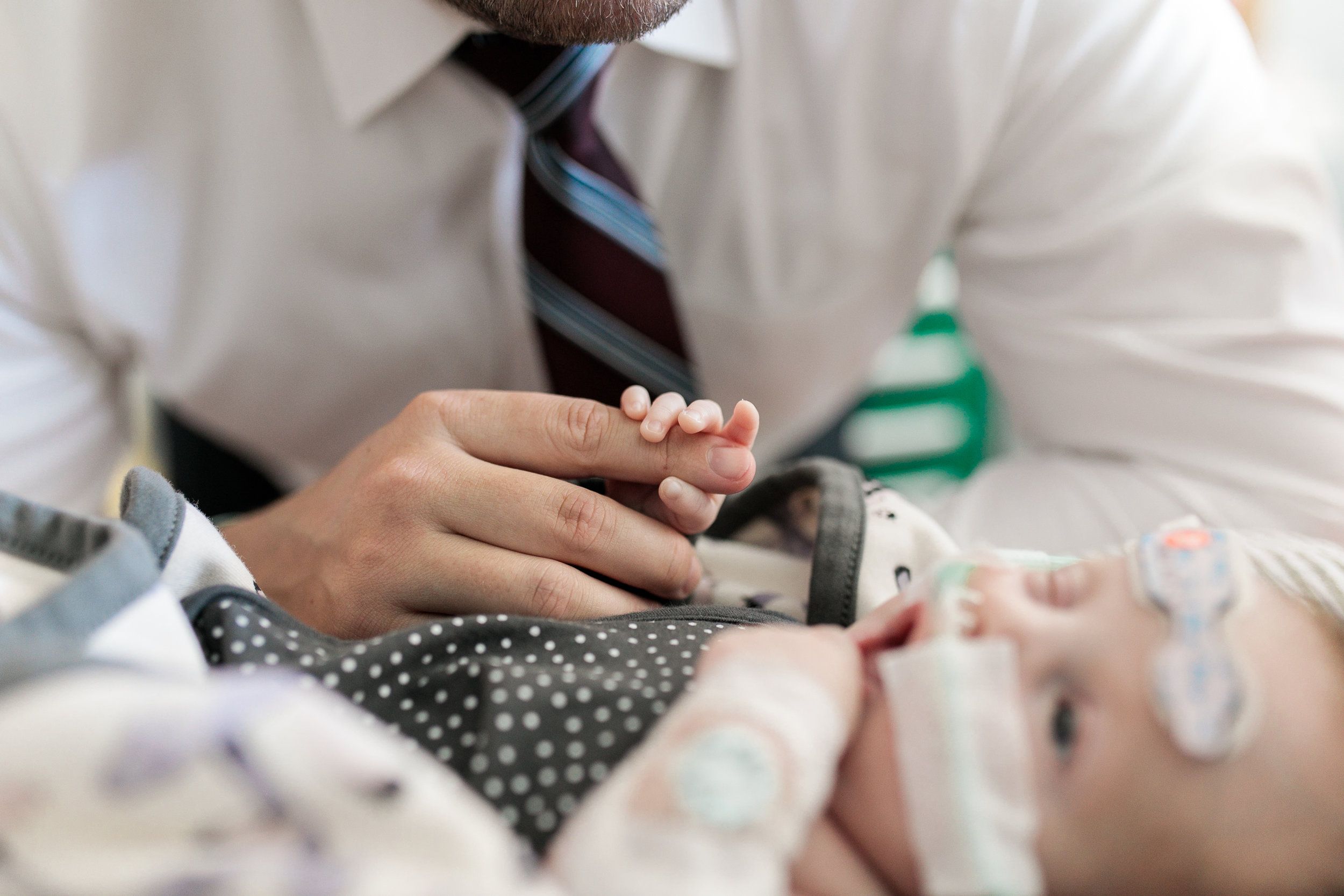
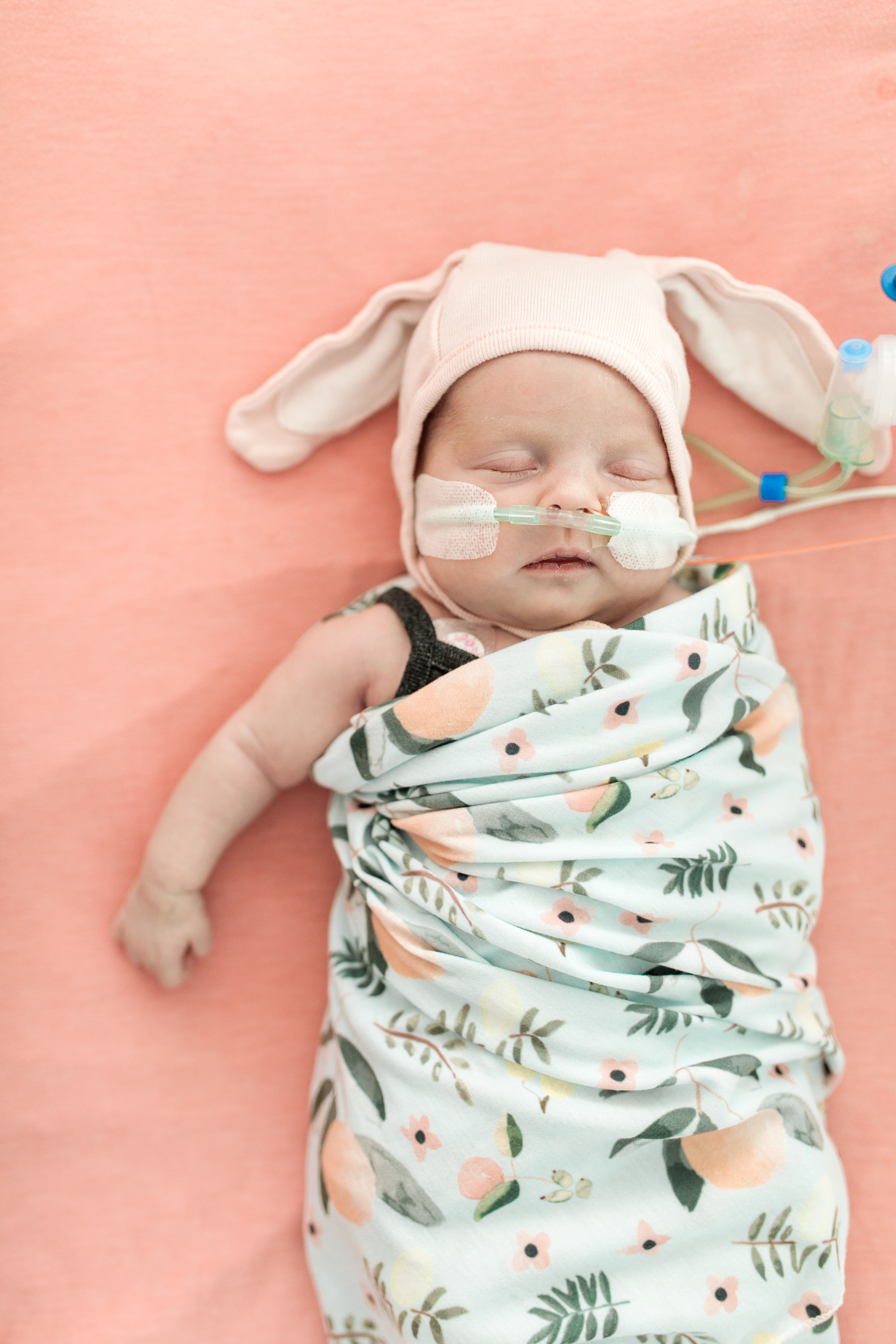
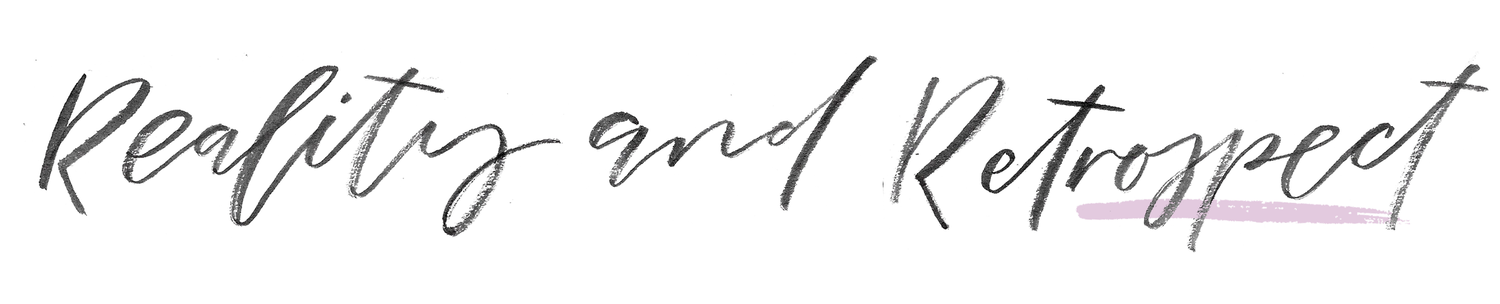Cecelia Faye's NICU Diary.
/Hey, guess what! We had a baby!! I’m guessing there are some of you who read the blog that don’t see my updates on Instagram. Cecelia Faye Jarman was born on September 30, 2017, and is the most perfect blue eyed, chubby-cheeked, mohawked baby girl that ever existed.
However, about an hour after she was born, she was taken down to the NICU for what I thought was a routine suctioning. It wasn’t. And it turned out to change our lives forever. Cecelia spent 51 days of ups-and-downs in the NICU. We’ve all heard that breastfeeding is best for newborns, but I learned it’s especially important for babies in the NICU. Thankfully, I was able to pump and produce enough milk for her the entire time, but there are so many moms who struggle with supply issues (especially when they are exclusively pumping!).
Having breastmilk is SO important for these medically fragile babies. That’s why I’ve decided to partner with Prolacta Bioscience on this sponsored post to raise awareness about the use of a human milk fortifier in the NICU. It’s something that’s added to your milk or donor milk in the NICU to give these fragile babies the added calories and nutrients they need. But the name “human milk fortifier” is confusing because most are made from cow milk! But not Prolacta’s. Learn more with this infographic.
Prolacta’s human milk fortifier is made from 100% human milk donated by mamas who have excess breast milk. It’s important to know that cow milk-based fortifier can cause several dangerous complications for preemies (read more here, here and here). If you’re a NICU parent like me, or have family or friends who are, be sure to share this or tag them in the comments below so they can learn more about the benefits of fortifier made with 100% human milk instead of cow milk for their baby!
If you are interested in hearing a little bit more about Cecelia’s birth and want to read my full NICU journal, feel free to see the following that shares all of our crazy highs and lows during her first couple of months!
Cece's birth story
Having babies isn’t that scary to me. It is just so exciting and I feel like I have so much energy and anticipation running through my body that looking back on them I don’t remember the hard parts much. On a Friday morning I was facetiming my mom at about 9 AM (like usual) and my water broke! I am still shocked that it happened that way. I was set to be induced on October 3rd and did not have my hopes up for going early after I was so disappointed I didn’t go early with Jay. I called Jarman and told him and he literally drove 100 MPH home from work and came through the door crying. It was hilarious. In the meantime, I was getting ready and making arrangements for Jay and not really even feeling contractions so I knew we didn’t need to rush much.
We got to the hospital and got checked in. I think I was at a 3 when we got there but I honestly can’t remember. My first L&D nurse was actually one that I had had when I was sick in triage one of the times during my pregnancy. I loved her and tried so hard to get my baby out before she left because I knew I trusted her. She was off at 4 and I told her my goal was to get Cece out before then and she said it would be a stretch but we would try! I wasn’t having many contractions at all so I got started on pitocin right away. My contractions would start to get worse so they would decrease the pitocin but then they would fade again so I had to have it my entire labor. Things moved SUPER slow. I tried to time my epidural perfectly to where it wouldn’t slow down my progression but also didn’t want to go past the point of not being able to get it. I got it before my first nurse left and I remember hugging her so tight during it and feeling so grateful that she was there. After shift change we watched Grease and La La Land (both major wins) and things slowly got worse and worse pain wise. I remember thinking that I didn’t remember the contractions hurting as bad as they did with Jay but these ones I couldn’t even talk through.
I got to about an 8 and my mom and Sydney came over to hang out just in time to see me throw up twice. It was so weird I felt totally fine and then it came on all of a sudden and luckily I had enough time to ask for a bag. Soon after that I felt ready to push. My doctor was delivering another baby so they wanted me to wait till she was available. Not pushing for about 30 minutes when all your body is telling you to do is push is SO hard. I feel like I was crying asking to push and they wouldn’t let me but that may be an exaggeration.
When the doctor finally came in I did 3 pushes and she came out! I couldn’t believe how fast it went. Pushing a baby out is the weirdest feeling in the whole world. It’s not painful as much as it is relieving. They laid her on my chest and I cried way more with her than I did with Jay. I couldn’t believe she was actually here after we had waited so long for her. I remember just hugging her so tightly and I couldn’t figure out why I felt so relieved to be holding and so happy that she was here. Jarman cried a ton more too.
She was kind of gunky coughing a bit but it didn’t seem like a big deal. They took her to the warmer to try to deep suction her but couldn’t get the tube down very far so Jarman brought her back to me and I held her a bit longer. The walk from the warmer to bring her to me was the only time he got to hold her that night. She kept doing a gunky cough so they decided to take her down to the NICU to try and suction again. I think my stress level at that point was about a 2. I literally just thought it was a routine thing and would be no big deal. Jarman went down with her and I stupidly tried to eat some pasta which I puked right back up almost instantly.
Since Jarman and Cece were downstairs all I wanted to do was look at my pictures of her from the little time we spent together. I uploaded them to my computer and was editing them when I started getting some scary texts from Jarman. First he said, “She doesn’t have a butthole.” I was literally cracking up at why would he use the word butthole?? Like who even uses that word. And I just kept thinking that they could just poke it through and it would be fine? Then we were texting and he told me there were two issues, first her butthole then her esophagus and that we would talk to the surgeon and find out more later. I asked him if things were actually scary (I was starting to worry a lot now) and he said they’d probably be fine.
About two hours after I had her I got rolled down the the NICU in a wheelchair. Jarman had already been down there for an hour with her and was sitting down signing paperwork and looking completely stunned. There were honestly about 7 nurses and drs running around doing things to her and getting ready to put in her umbilical line. The first person I talked to was a girl who I recognized. We put it together that she was in our ward (what are the odds??). I was sitting in my wheelchair next to Jarman and she started telling me the list of issues. I hardly remember her words I just remember crying and looking at Jarman who had finally started to cry too. Looking back on it it felt like I was underwater seeing everything move around me and people trying to talk to me through the water but I couldn’t understand what they were saying except that there were lots of issues with my perfect baby girl. I went over to look at Cecelia and her arms were tethered above her head- she was strapped down for the little procedure they were about to do and it was the saddest thing I have ever seen.
They took me up to my recovery room and I don’t remember speaking to any of the nurses, just trying to control my sobs. I got up there and got help in to the bed. My last L&D nurse (who I actually ended up liking) gave me a big hug and actually cried with me for a minute and told me she would be praying for me. I had two nurses who were over my recovery. I’m not sure how much they knew but they were definitely a little too bubbly for the situation. On my way up I had mentioned that I’d want to go back down and see her again as soon as possible. They took that super literally and were almost trying to rush me back down there and I realized that I wasn’t quite ready yet. All I wanted was Jarman and I needed him to be there immediately. They called down and had him come up but it seriously took way too long.
When he finally got to my room he sat on my bed and I have never cried as hard as I did for that hour with him. I couldn’t even get words out I just couldn’t even understand how or why this was happening and if everything would be ok. I am so glad I had him at that time because he truly is the only person I wanted in those deepest moments of despair. Once we finally pulled ourselves together we laid down and actually slept for about an hour before we were ready to head back down.
We went down and met with Dr. Gollin for the first time and I felt so comforted. He took as much time as we needed to make sure we totally understood what was happening with Cecelia. Her first surgery would be the next day to combine the two pieces of her esophagus. We spent the day downstairs with her as much as we could. Jarman and my dad were probably back there the most sitting with her. In the evening we got to hold her for a little bit while Mandy did pictures and it was amazing. But we were so completely exhausted and had to wake up early the next day for surgery.
Cecelia Faye Jarman:
[[a compilation of my text updates I sent out to friends and family]]
October 1 6:44 AM
I had her at 3:30. She's going to be in the nicu for a couple of weeks she's got some scary things going on. She doesnt have an anus and her esophagus and stomach aren't attached. And she has some growths on her spine. There are a couple of different syndromes she could have so they are going to do more tests on her to see if there's anything else going on with her heart are kidneys. The surgeon is coming sometime before noon so we will know more then.
October 1 12:06 PM
Ok so we just got back from the nicu and are feeling lots better. We talked to the surgeon and have a lot more figured out. She has VACTERL syndrome. It's like an association of different things. It's an acronym you can look it up. She has four of the six signs. The first issue is that the top part of her esophagus just goes down and connects to nothing so she is on constant suction to get all of the saliva and fluids that are going down. The bottom part of her esophagus is connected to her trachea. Tomorrow she will have a surgery to take the two parts of the esophagus and attach them together. They'll go in through her side so she'll have a little scar. The second issue is that her anus and vagina are connected. During the surgery tomorrow they will give her a colostomy bag to collect her poop. She's too small to fix the issue right now there's not enough tissue down there to work with. So she'll have another surgery when she hits 12 pounds. She has a heart murmur because of a little hole in her heart but its nothing too serious at this point they don't plan on doing surgery or anything. And she has a growth on her spine which also isn't a big deal and they don't have plans to do anything about. So after the first surgery tomorrow the goal is to get her eating for real (right now she's getting nutrients through a line into her umbilical cord) and she should start that at about 5 days after the surgery. Then once she starts eating well enough she can come home until she is big enough for the next surgery. We can't hold her yet because of the umbilical line and the suction into her mouth but she has been totally calm and peaceful every time we've been down with her. All of her breathing and everything is really good. So it sucks but after talking to the surgeon we feel totally fine. And she will be fine and normal once we get these things fixed.
October 1 12:18 PM
We stopped crying so that's good!! It was pretty crazy when I went down there at first and Jarm was down there for a couple of hours with her and it was really hard. There were nurses and drs buzzing around and things were just a lot worse than they initially thought. I was only down for like 10 minutes but then came up to be checked and stuff and I just couldn't handle or comprehend all of it yet it was so hard. But after going last time we feel really good. My dad and Jarm will give her a blessing later today prob.
October 2 10:22 AM (TEF Surgery Day)
They called me at nine and were 10 mins in and it was going well! It'll be about 3 hours. Just got back to my room and am checking out soon hopefully. She'll be staying at rady's so we are just gonna go home today since we won't be super close
October 2 7:40 PM
So after her surgery we talked to the surgeon and he said that he was so happy because the two different pieces of her esophagus were totally long enough and there wasn't any stretching to stitch them together so that was really really good. We are lucky her top part of her esophagus even went down 11 cm. AND she didn't even have to get a colostomy bag!! Her anus was separate enough from her vagina that he was comfortable not doing that which means two less surgeries that she will need. We will have to do a probe to dilate her anus until she has a surgery when she gets big enough (between like 3-5 months). But she's already done a couple of normal poops today. So that was awesome too. Her breathing tube is still in but it's looking like she will be able to get it out tonight. They tried to give her a PICC line in one of her arms to feed all of her nutrients through that but were unsuccessful because her veins were so small but they'll try again tonight. I got checked out and went home to nap a bit and shower and see jay and eat and am back now. Jarman was here for a few hours with her while I was at home and has been so cute and knows everything about all her machines she is on❤️when I got here she was crying and so red but she can't make any noise because of her breathing tube so that was really sad to see but she's calm now.
October 2 4:40 PM
Hey guys! Cece is doing really well today! She has been resting a ton she got her picc line in last night and they ended up giving her morphine and something else so she was sedated pretty heavily and still hasn’t woken up. But her breathing is great they are planning to take out her breathing tube soon! She has had a couple of X-rays and things are looking good. And she actually does have an anus separate from her vagina, it’s just really small and really close. But it’s a separate hole which is awesome. I learned how to do her ‘dilating’ today which we will have to do until she can have surgery to make it even more separate and it wasn’t as bad as I though. And she has been pooping really well. Her urine output is a little concerning but they are thinking that it’s just all the medication she is on. We spent a lot of time with her this morning and afternoon and are heading back for a few hours this evening. I got to speak with her surgeon and NICU attending for a while and they are both AWESOME and so helpful and nice. We have been getting all of our questions answered which have been a ton.
October 3rd 5:55 PM
Cece’s update for the day: We’ve had some ups and downs today. The best thing is that we got to take out her breathing tube and see her pretty face again❤️❤️ it was the most exciting thing ever. Her blood is showing that she may be getting an infection so they started antibiotics until we get results from her cultures to determine whether or not she is. She has been so much more active today and we got to see her open her pretty eyes for a while. She got a second echocardiogram to check on her heart. The cardiologist came back to talk to us and we got some scary news. The hole in her heart is bigger than they originally led us to believe. There is an over 50% chance that she’ll need open heart surgery between 3 and 6 months to patch up the hole. There’s still a slight chance that she won’t need the surgery if the size of the hole goes down a bit- so I’m officially praying for a miracle for that to happen. The hole in her heart means that she will be getting too much blood to her lungs making her breathing more labored and it will make it harder to gain weight. Luckily if she does need the surgery it is pretty routine with minor risks.
October 4th 1:03 PM
Cece update: She has been pretty active today which is so good- she gets super mad with everyone bugging her and poking and prodding all the time but that’s a good thing compared to how sedated she was before. We found out that she has an infection E. coli in her blood which means she’ll have to be on antibiotics for 10-14 days. Luckily they caught it early and started treating her right away. She now has an infectious diseases dr following her case- this is her fourth dr that is watching her carefully😂🙌🏽😭 they are going to check her CSF too which means she basically has to get an epidural just to make sure the infection hasn’t crossed in to her spine/brain. Which would mean she has meningitis. They are just ruling it out. The antibiotics she is on treats that too and if she does have it she would just have to have a longer treatment. Crossing our fingers she doesn’t. We talked with one of her other drs about her heart issues and luckily she isn’t showing symptoms yet. He is going to meet with the cardiologist and come back and talk to us a little later. But the best news is that she is getting her umbilical line out today which means I will probably get to hold her for a bit!!! ❤️❤️❤️ I’m really just amazed at how on top of everything all of her drs are- we are so lucky to be at the hospital and to live so close!
October 5th 5:28 PM
Today has been really good!! No bad news so far! Her bacteria cultures came back all negative from yesterday, and so did her CSF culture. They’ll keep following it for a few days to see if it develops anything but so far so good. So we are doing antibiotics for 10 days from her last positive culture which was yesterday, which puts us at 10/13 as the earliest for going home. The other factor will be how well she is eating. Tomorrow is her dye test where they have her drink blue dye and watch on an x ray to see where it goes and make sure there are no leaks in her esophagus and that nothing comes out of her chest tube. After that we will try a bottle and see how she tolerates it. So tomorrow is a really big day for us!!! We tried taking out her nasal cannula that is giving her air but put it back in because she wasn’t quite ready, but that’s ok we have plenty of time for that. I asked them to recheck her kidneys because part of her VACTERL association is kidney issues and we want to be sure they caught everything. They were working on that when we left the hospital.
October 6th 6:04 PM
Cece is killing it today!! She hit three major milestones. 1. She did the dye test while being x-rated and we saw all of the dye go down her esophagus and in to her belly with no leaks. She did SO well drinking the dye (her first thing she’s ever eaten) and didn’t even get too upset with all of the different ways they were moving her. 2. She drank her first real bottle! 10 mls of mommas milk. It took a few tries to get her to take it but eventually she did it and kept it all down. This meant that 3. She got her chest tube out! The drs keep saying how painful the chest tube is but her surgeon wanted to leave it in until she passed the dye test and got her first bottle. She did really well when he came in and took it out though. She has had a couple of crying fits today and turned blue twice😬😳😭😭 but it was because we were agitating her and we were all right there so it was fixed right away. Her breathing is doing better with her nasal cannula back it, but her dr wants it out pretty soon so we will start weaning off of it soon. The infectious diseases drs came by and checked her out and her last two cultures have still been negative... but they said that her antibiotics need to run for 14 days instead of the 10 that we originally thought- putting us at October17th. Her incision from surgery has been oozing a bit but we have had three different drs come and look at it and none are worried. With her chest tube out holding her can be a more regular thing! And now we will get to feed her every three hours and work our way up to 60 mls before we get to go home. We should have plenty of time to make that happen.
October 7th 7:59 PM
Today was fairly uneventful which was much needed after the chaos yesterday. She was refusing to eat, or breathing too fast to eat for a lot of her attempts at feeding yesterday but overnight the nurse got her to eat a little bit at 3 and 6. Which was such a tease because she ended up not being allowed to eat today. Her X-ray showed some extra fluid around her incision site and her lung was partially deflated so they put her on a cpap machine to help fix those problems. The dr didn’t seem too concerned and said it was normal after pulling out a chest tube. She had a repeat X-ray at 6 pm (which we haven’t gotten the results to yet) and will have one tomorrow morning if this evenings wasn’t improved. She was pretty fussy this morning and seemed like she wanted to eat, but she settled after a dose of morphine and let Grammy and Dad hold her for a while! Hopefully we can take her off the cpap machine tomorrow and start working on feeds again.
October 8th 8:21 PM
Cece had to be on the cpap machine today still because her X-ray showed fluid in her lungs. It had improved from yesterday but had also moved more to the left. They started cardio physical therapy to help get the stuff out of her chest (basically a little machine that vibrates to help it move). Her white blood count and CBC was a little elevated so she started getting another antibiotic just to be on the safe side, and we redid her cultures. She was SO much more content today and just seemed like she felt better and didn’t get so agitated when we had to bug her with all of the things. Her breathing is still pretty fast but hopefully that regulates once she gets that fluid out of her chest. I got to help give her a little sponge bath which was so fun and she only hated it a little bit😉 hopefully we get her off cpap and starting feeds tomorrow!
October 9th 7:35 PM
Cece was so happy and content today! They decided to slowly wean off the cpap so still no eating but she is down to a lower setting. Tomorrow they’ll go a little lower and see how she does. Her surgeon came in to see her and said she is doing exceedingly well for being 8 days post surgery and 9 days old❤️ her incision is splitting a little bit in the back where the glue has come off and it looks kind of freaky but I have had every dr look at it and none are concerned- it’s not infected and it’s surface level so it’s not a big worry. Andie and Grandma Karen got to hold for the first time today!
October 10th 9:58 PM
Today was a hard one. We finally put it together that the odds of us going home anytime soon are getting smaller and smaller. Cece is doing good and has been off tylenol for two days now and seems to be mostly happy. But her respiratory rate is still too high to take her off cpap or start feeds any time soon. Since she has so many things going on they aren’t sure what is making her breathe so fast- it could be that she is still recovering from her surgery, or her blood infection, or her heart issues. They started her on a new medication for her heart and gave her a blood transfusion today because her red blood cell count was low and babies don’t make their own RBCs until they are 4-6 weeks old. The drs didn’t seem too concerned about her needing a blood transfusion it definitely sounds scarier than it is. And her new heart medication is supposed to work with the diuretic she is on to help everything work more efficiently and hopefully not send too much blood to her lungs. We were originally told 2-3 weeks to go home but that was before we knew how serious her heart issue was so that is just adding it’s own set of obstacles to getting us home. It’s getting harder and harder to leave her! Thank you all for your prayers❤️❤️ feel free to text me individually if you want to respond.
October 12th 10:58 PM
Sorry I missed yesterday and this one is coming so late! Things have been pretty stagnant over here while we figure out cece’s breathing. She is still breathing way too fast to eat most of the time so until we can manage that things won’t change much. She got put on a new heart medication and they increased the diuretics she is on in hopes that they can medically manage her breathing/heart issues. They still aren’t 100% sure that she is breathing so fast because of her heart it could be because she is still post surgery or because she has the bacterial infection. Dr came by yesterday and said to plan on about a month longer in the nicu, which we had figured after talking to someone else yesterday but it definitely made it more real. So today we moved in a little bit more-‘brought over all of her blankets to dress her crib, got our space all organized and are planning to be here for longer than we had hoped. She had an ultrasound of her brain last night which is standard practice for ‘cardiac kids’ and super stressed me out but it came back totally normal- we are pretty sure she’s gonna be a genius with all of the dr talk she is gleaning right now. Her X-ray this morning showed not much improvement in the fluid in her lungs so hopefully the extra diuretics helps to move that along. Her dr also got her favorite pediatric cardiac surgeon to take our case and should be coming by to meet us and talk game plan soon. They still want to get us home before she has the heart surgery. She has been pretty happy lately though and I got my first real smile with her looking right at me yesterday!! Can’t believe she is already 13 days old!!!
October 13th 8:40 PM
Cecelia had a busy day❤️ since things have remained pretty much stagnant for a week now with her breathing still being too fast to eat the drs are looking at other options to help her. They all pretty much agree that the breathing is because of the large hole in her heart (a VSD if you wanna look it up). Since they have her on the highest dose of the heart medicine (Milrinone) to help her heart Work more efficiently, and they have her on diuretics to help flush out the excess fluids and both of those things aren’t working they need to take more steps to fix the problem. They are increasing her CPAP from a 7 to an 8 (not really sure what the numbers mean but 8 is the highest) and they are adding nitrogen in so that she is getting a little less oxygen. They are thinking what will help her to not overcirculate like she has been is another surgery. It’s called pulmonary artery banding or a PA band. They go in and put a band around the pulmonary artery to physically restrict the amount of blood that goes to her lungs so that she won’t have to work as hard to breath because of the extra blood. This would help to get her more healthy before her actual VSD repair which is an open heart surgery. They want her to be as healthy as possible for that surgery and are hoping to buy some more time to do so with the PA band. I was hesitant when the first person came and talked to me about that and was so annoyed we had to change her CPAP back to an 8 because it feels like going back a step. But after talking to a few different drs and the cardiologist it seems like the right thing to do. They definitely don’t take these decisions lightly though- on Tuesday they are having a meeting with all 20’of the cardiologists and heart surgeons to discuss her case and figure out the best plan of action. We also officially have a heart surgeon who is super experienced and amazing and is actually married to one of her NICU doctors. Dr. Lamberti is his name and everyone says he is the best. We are excited to meet with him soon and talk to him. In other news we finally got a room with a window since we are in this for the long haul. And jay came back to see Cece for the second time (the first was a disaster) and was adorable and gave her hand kisses and wasn’t freaked out at all😍 he kept asking to give her a bottle ironically because that is what we all wish we could do!
October 15th 9:08 PM
This weekend has been pretty low key for Cece. They added nitrogen in to her cpap so that she is getting a little less oxygen making her circulate less. It sounds counterintuitive and scary but it actually seems to be helping her oxygen sats decrease (which is good for her heart condition) and her breathing is starting to slow down a bit too! They also added in an extra dose of diuretics every day to help with those issues as well. But obviously these are only temporary solutions because we can’t take her home with a cpap machine. So now it’s just a waiting game till the cardiac conference where they will discuss her case. Her heart surgeon will be the ultimate decision maker. Her dr said if her breathing stays as good as it was today we can have the occupational therapist come tomorrow or the next day to determine if she is doing well enough to try some small feeds. Trying to not get my hopes up because obviously I have thought ‘tomorrow’ was going to be our day to feed her quite a few times now. But I was excited when she said that!
October 17th 9:07 PM
Yesterday Cece an NG tube (feeding tube in her nose) which for some reason seemed stressful and scary to me but is actually a really good thing. They wanted to start giving her real food (breast milk) to see how her tummy handles it and make sure she digests well. Normally a nurse would just do it bedside but we had to take her to radiology so that they could do it under X-ray because they wanted to be super careful with her esophagus because of her surgery. She cried the whole way to radiology, during the whole procedure, and the whole way back! Which is legitimately the most she has ever cried. She still struggles with figuring out was to do with her spit/secretions when she cried so last night she was super gunky and kept spitting up spit and phlegm. Today was the cardiac conference but they still haven’t come to a final decision on the plan for her case. They requested her to have another echocardiogram to follow up, and wanted to make sure her incision from her last surgery and infection are healed well enough. They might want to do a CT of her chest as well. Hopefully they will look everything over and have a decision by the end of this week. She has been getting feedings through the NG tube and is handling it really well! She started on 5 mls every 3 hours and is going up 2 mls every 12 hours until she gets to a full feed which is 60 mls. She had a bunch of labs done today (well she does every day but there were extra ones today), and she had the wounds care dr and occupational therapist come look at her. So she is exhausted now to say the least. I came back to cuddle a little bit more because I’m pretty sure she sleeps best in my arms😉❤️
October 19th 7:19 PM
We are still stuck in a waiting game and probably will be for the next couple of weeks. I finally met Cece’s heart surgeon today and got to talk to him for a while. (He’s literally Mr. Feeney from boy meets world- but everyone says he is the BEST and most experienced so we are so happy to have him). He said he would prefer to do the VSD repair over PA banding- but the banding is less risky. There are so many factors that are going in to the decision of when to have so the surgery. She just had surgery on her esophagus and trachea so intubating her again is going to be tricky. Plus she can’t be deep suctioned from her last surgery still which is typically something they need to be able to do. As of right now she is gaining weight and is stable so the surgery isn’t super urgent- but he said that could change and push him in to surgery. Plus he obviously wants her to be bigger even though they can do it at her size. So he just mainly said that he’s really thinking it through and waiting for a sign of when it’s go time. I definitely don’t want him to rush it as much as we want to get out of here. He also has ordered some other tests to make sure she is as ready as she can be for open heart surgery. She had her echo a couple of days ago and today she had a chest CT and all of her drs looked at her incision because they were worried about it dehiscing but it still looks good and like it’s healing. So if I don’t send updates every day it’s just because we are kind of at a stand still! But her feedings with the NG tube are going really well and she’s pooping again after not pooping for a while. So that’s pretty exciting for us🙌🏽
October 20th 7:23 PM
Cece’s CT scan from yesterday showed that her trachea has some narrowing that the cardiac surgeons are worried about. They asked the ear nose and throat specialist to look at her (one more dr to add to her growing list). So next week she will be getting a Bronchoscopy where they put a camera down her trachea to see what is causing the narrowing and if it needs some sort of intervention or surgery. She’ll have to go to the OR and be put under anesthesia for that. If she does have to have some sort of surgery they would do it at the same time as her heart surgery since they will have to open her chest for both. But they won’t really know any details until the Bronchoscopy so hopefully it’s just nothing to worry about. A couple of days ago she had an elevated hormone from her pituitary gland so they had a endocrinologist look over everything because the neonatologist wasn’t sure how to interpret it. But luckily that was ok - just another dr looking at her. Her breathing has been a little raspy from crying so much yesterday but it’s gotten better throughout the day. She had the occupational therapist come in today and give her a little baby massage and she LOVED it. I was dying she was awake the whole time and sighing and so in to it. And then she got a bath and has been sleeping ever since❤️ so tuckered out!
October 22nd 4:48 PM
Cecelia has been having a really rough day. This morning I woke up with a call from the nurse practitioner (which has never happened before so I knew it was bad) saying that her breathing was really labored and that they needed to make a few adjustments. The increased her cpap, changed the cpap machine to this crazy one that basically covers her whole face, switched her from nitrogen to helium (which helps distribute her air more evenly without overcirculating), gave her some pain meds, gave her a nebulizer to help her airway and are starting some steroids to help her airway. Apparently her trachea is a much bigger problem than they originally thought. It narrows to about the size of a coffee straw and so that is what’s causing the issue along with her heart problems. They think that since her feeds were increasing she maybe had a little bit of reflux because of her esophagus surgery and so that pushed her over the edge from being stable. And that her fast breathing that she was struggling with (which has actually gotten better) was a combination of trachea and heart problems. She’s still struggling with her breathing- it’s super labored and you can see her chest really working with each breath- but they are doing everything they can to not have to intubate her because that is the last thing she needs. Basically they are trying to keep her stable over night until the ENT dr they want to see her comes back from vacation which should be tomorrow. There are other ENTs on call in case it gets worse but the one they want specializes in cardiac babies. We won’t really know her plan surgery wise until he comes and they do the Bronchoscopy. Her poor face is swelling up too from the pressure of the cpap increasing. She just looks so miserable and cried so much this morning until she got the pain meds. Thankfully the nurse practitioner who has seen her a lot this week was here and has been in our room a lot today, our nurse today is awesome, and she has almost had the respiratory therapist to herself. It has been really scary but she is going to be ok.
October 23rd 7:20 PM
I spent my first night with Cece in the hospital last night! I did NOT want to wake up to another scary call and since her day was so hard I was worried about her night. The drs decided to take her off helium/nitrogen and to just give her all oxygen and that helped a lot. She was going so up and down with her oxygen saturation before that but since then she has been pretty stable. She is still getting a lot of pain meds because she is struggling with breathing so much especially when she wakes up and moves around and because of her giant cpap machine on her face. The goal for the past two days has just been to keep her comfortable and happy as possible. The ENT’s fellow came this morning basically just to say her bronchoscopy would be tomorrow morning at 11:30 and to get the consent forms signed. So today has just been more waiting to get her to that procedure. I am so anxious to see what the plan will be once they take a look at her trachea to see what’s going on. But overall today has been better than yesterday and she has been more calm and relaxed. I’m staying with her overnight again and don’t know how I’m ever not going to after our scare yesterday morning!
October 24th 2:00PM
I’m still trying to process everything that happened during the bronchoscopy. This might be the longest update evs- sorry about that! So first they went down with a scope and immediately saw what the problem was that was causing her breathing to be so labored. There was a spot towards the top of her trachea that had scar tissue from when she was intubated during her last surgery. It had closed up and was about the size of a pin hole. The dr knew that he needed to do something immediately so he put a balloon type thing down to expand that portion of her airway and it worked really well. He said that scar tissues happens sometimes randomly after intubation and there is no way to know beforehand or prevent it. So they are planning to keep a very close eye on that and will probably be doing more bronchoscopies to watch and make sure it doesn’t happen again - especially since she is intubated right now after that procedure and will have to be intubated for all of her surgeries. Next they saw that the bottom part of the trachea is very floppy and collapses every time she breaths in. It’s called tracheomalacia and kids who have the trachea-esophageal fistula that she had always have it, but hers is worse than most. So that may need to be repaired which would likely happen at the same time as her heart surgery. Last they found that the part which is supposed close the trachea off from food when you eat is lower than it should be. So when she eats or drinks it can easily go in to her trachea. This puts her at a big risk for aspiration. That will definitely need to be repaired too. It’s called a larygnotracheal cleft (LTC). Until that gets fixed she can’t eat orally. They think it will be best for her to get a g-tube to feed her right in to her stomach since she will be here for so long. The LTC repair will have to be her very last surgery because they won’t want to intubate her for months after that because it would affect it. Since she has so many different surgeries that will need to happen she will have the g-tube in for a while. The ENT dr described her as a 1,000 piece puzzle and all of her different problems make her case not super straightforward. We still don’t have a set plan for her and probably won’t because it will just depend on how she is doing. All of her surgeons (cardiac, ENT, and general) will meet to discuss and hash out her case to figure out what needs to happen first. The ENT said that we definitely won’t be out by Christmas. So we just really need to start getting used to being patient and not really having a plan for her and just seeing how everything goes. Remember how I wanted to be induced so that I could have everything perfectly planned out??? Apparently HF is telling me to chill out a bit😉 The good news is that after opening up her airway she looks so much more comfortable and is doing a lot better. When we got in this morning I could hardly be in the room with her because it was so hard to see her struggling to breath so much. She looks so much better now. We are just waiting for her to wake up from the anesthesia so that they can extubate and I can cuddle her- it’s been a few days now!!
October 25th, 2017 6:02 PM
Today has been SO good! Cece looks amazing- better than ever now that she can breath normally. She looks like a completely different baby compared to yesterday morning. We gave her a good bath after a long weekend with no baths- of course she loved it. She had kind of a rough night last night but they got her pain meds figured out so that she could rest and actually stop the pain meds this afternoon and she has done great. They pushed her NG tube in a little bit further so that it goes right in to her intestine so that hopefully she doesn’t have reflux as much and started her feeds. A few of her drs are hopeful that she can get off of the cpap soon (she’s already on a lower setting than she ever was before), and then once she gets her g tube and is getting full feeds there is a possibility we might get to go home before her heart surgery!! We are trying really hard to not get our hopes up too much because obviously things can change really quickly- but if she stays as good as she is today we might be lucky! The good news is that her fast breathing over the past couple of weeks is likely due to her trachea problem not her heart problem like they were thinking. And now that it’s fixed she can breath better. Her ENT thinks there is a good chance it could close up again but maybe it won’t. Her next big day is going to be next Tuesday. She is going to go down for another bronchoscopy to see if anything changed since they fixed the spot in her trachea. And the cardiac team will be meeting to discuss whether or not they should do the heart surgery before the g-tube surgery or after. They want to look everything over really closely to make the best decision. Hopefully her breathing doesn’t change too much before then!!
These are the before and after pics of her trachea. And think about how small she is and that these are blown up quite a bit. The dr said it was literally a pin hole and he doesn’t know how she managed for so long. If she had any sort of gunk go down there it could have completely blocked her airway! So glad the balloon catheter was able to fix it so easily and praying that it doesn’t happen again!
October 27th, 2017 9:50 PM
The past two days have been about as good as they can be when your baby is in the nicu. Cece is off all pain meds after her bronchoscopy and has been breathing so well. She even got off CPAP and switched to nasal cannula (hoping to wean that soon as well). She also got the stickers off her head and kidney that were measuring her oxygen since she’s not on nitrogen anymore (I begged three different drs yesterday to make that happen😂). She has been waking up more and actually has the energy to cry (even though she still hardly does). Today I saw her startle for the first time like a real baby- I forgot babies do that all the time! I talked to her ENT surgeon and he said she is a hot topic around the hospital and that there are different camps on what direction they should go with her. It’s sounding like they are leaning towards waiting to do the heart surgery. As long as her breathing doesn’t change too much she might be able to get her g tube next week and then once she is up to full feeds on that we could potentially go home before her next surgeries. That’s of course in a perfect world if nothing goes wrong but I feel like we kind of deserve that to happen at this point after so much going wrong over the past month. So we are just waiting for next Tuesday still!!
October 30th, 2017 9:56 PM
The past few days have been really good for Cece! She has been waking up more but sleeping really well at night (she did 8-4 last night! Hoping she’s sleep trained by the time she gets home😉). They have been slowly increasing her feeds and she just hit her goal of 20 mls per hour. They do it gradually so that she doesn’t react to having so much in her belly. She is still on a constant drip so that her belly doesn’t get too full all at once. Tomorrow is our next big day! There is another cardiac conference to discuss her timeline for heart surgery and her other surgeries. Since it is looking like her breathing issues were trachea related instead of heart related they are tentatively planning to wait on doing the heart surgery. They will decide for sure (ish) tomorrow. Then She is having another bronchoscopy to check and see if the scar tissue is growing back. Her breathing has stayed super stable though so hopefully that means that they won’t have to fix it again. I signed a consent for to let them do laser, balloon catheter and steroids if they think she needs it but the ENT is hoping to leave it be. Since she will be under anesthesia her other surgeon said he might as well do the g tube surgery as well. So she will be getting that put in tomorrow too. It conservatively takes 2-3 weeks for them to recover from that and get up to full feeds so there is a good chance we could be going home that soon😬😬🙌🏽🙌🏽😭😭😍😍
November 1st, 2017 11:51 AM
Cece’s surgery went really well yesterday! The ENT didn’t have to do anything to her trachea the scar tissue hadn’t grown back. He was surprised at how good it looked. And she got her g tube in and has already started feeds on it! They extubated her before she even came back up to her room and she was already awake and everything.
November 1st, 2017 9:15 PM
Today has been a little rough. Cece is recovering from her surgery yesterday and has been pretty uncomfortable and fussy. She has been getting Tylenol and morphine every few hours but is still pretty unsettled. She had a little fever for a bit and was coughing and having a harder time breathing and desatting so I was freaking out- but she actually has settled down and looks a lot more comfortable. They are running some blood cultures and checking for RSV just to be safe. And she had a chest X-ray which showed one of her lungs was a little deflated and she had some more fluid in there than usual. And her RBC count was low so she is getting a blood transfusion which meant she had to get another IV line in her hand🙄 soooo I’m really not sure what all of that means. Hoping to get negative cultures back tomorrow and that she is just not feeling well from surgery not from another infection. Plus her nurse today was 😑😤🤢😷... we didn’t like her to say the least. But Jarman brought down the hammer and fixed that so we have an awesome night nurse and won’t have her again. Cece just needs a good stretch of sleep to feel better I’m sure!
November 2nd, 2017 9:29 PM
Much better day today! All of cece’s culture have come back negative and she seemed to be feeling a ton better. She was still pretty sleepy but when she woke up she was looking me and Jarman in the eyes non stop😍😍 she got a little sponge bath which I’m sure made her feel better too😉 we had a long chat with the cardiologist about the plan for her because some of the NICU Drs kept telling us her heart surgery would be in 2-3 weeks which we knew wasn’t likely. They misinterpreted- they will be discussing her case again in 2-3 weeks. If she is showing signs that she needs the heart surgery they could do it then, but if she is gaining weight and doing well with the g tube, and if her airway stays as good then she would hopefully go home to grow before surgery. It’s so hard to have so many different scenarios and what ifs when it’s all going to be up to Cece in the end. Of course the drs are going to do what she needs but we don’t have a crystal ball to figure out what’s gonna happen (one of her surgeons uses that phrase a lot😂). G tube feed are going well so far she hasn’t had any spit up or gagging episodes and should be up to the full amount by the end of tomorrow. She’s getting a constant drip and her goal is 20 mls per hour (she’s currently at 14). The g tube is definitely a little more intense than I had worked up in my head and is going to take some adjustment- but I’m sure in a week it’ll seem like no big deal😬 I have been avoiding the internet but wish I would have researched that a bit more to be more prepared. Thanks for listening to my long updates- this is basically the way I’m journaling this whole thing so I try to include as much as I can even if it’s not super important.
November 6th, 2017 9:56 PM
Cece had a really good weekend! She is up to her full feeds and is getting all of her food in her belly now- no more TPN (baby Gatorade) in her IV🙌🏽. She is still on a constant drip but we are starting to condense her feeds during the day. Each day we are going to shorten the feed by half an hour- so right now she’s getting 1 ‘bottle’ over 3 hours every three hours (constant) and tomorrow she will get on bottle over 2.5 hours then have a 30 minute break. The goal is to get down to 1 hour so she doesn’t have to be hooked up to the pump all day long. I️ pulled her NICU dr in to talk about everything we need to do to get her home. First is working on condensing feeds. Second is weaning her nasal cannula levels (right now she’s not getting extra oxygen just flow which is helping her lungs- the dr thinks this might be our biggest holdup in going home but I️ think she will do great). We also have to get all of her meds to be oral instead of iv. She will go home on 1 or 2 diuretics and then another prescription for her heart and reflux medicine. If everything goes well with the bronch tomorrow and she does well weaning off the air and working on feeds then the earliest we could go Home is next Wednesday or Thursday. Of course that’s in a perfect world with not one hitch. I️ wish I️ could help her and do it all for her but really it’s all up to her- so much pressure on a baby😂😬🙈. She had an X-ray this morning which showed a little bit more fluid in her lungs than her last one and her dr thinks it’s cuz they stopped on of her diuretics. I️ asked her if besides that X-ray she is showing signs that she will need heart surgery sooner rather than later and she said as of right now no, but she is getting a lot of help from the nasal cannula and the meds so it could change. I️ have a feeling her bronch is going to go really well tomorrow because her breathing has been good. Hopefully I’m right!! It’s not until 4:10 tomorrow so we get to wait allllll day long. I️ kept telling my mom that Cece is getting bored in the hospital and needs to be stimulated more but she said it’s probably just me that’s getting bored😂 I️ think this might be the hardest week because it seems like she is good enough to go home and I️ just am getting super antsy to get her out!!
November 7th, 2017 7:28 PM
Cece’s bronch went pretty well today. Her ENT said he was happy with how things were looking, but it had changed a little bit from last week. You can see some of the scar tissue getting a little worse. He said since she looks so good and is doing so good he didn’t want to rock the boat and make it mad by doing anything too it. He could have gone either way though and done steroids or another catheter but he said if it were his kid he would have left it alone too. He wants to see how it looks/changes/evolves next week so she’ll have to have another one next Thursday. So of course this is our first hitch in getting out ASAP. He still wants us to go home and thinks we will be able to soon. She wasn’t able to eat all day because of her procedure and she was definitely hungry poor baby. And she was pretty mad when she got back but once she got some IV Tylenol she has been resting since. She’ll start getting food again tonight! Next steps are slowly making the changes- condensing feeds over the next few days and switching her meds to oral. Her dr doesn’t want to start weaning her nasal cannula till Monday because she doesn’t want to do too much at once and that will probably take a while. And then cardiac conference on next Tuesday and bronch next Thursday. So it’s going to be a long slow week over here! Which is good for Cece but makes us impatient😂
November 12th, 2017 9:31 PM
So everyone in the NICU is acting like we are heading home soon!! I️ am trying to not get my hopes up too high but I️ really think it’ll be before thanksgiving 🙌🏽 since her bronch last Tuesday she has been doing really well. Her breathing hasn’t changed and she looks super good and healthy. She has gotten all of her meds switched from IV over to oral (g tube meds) which is one of the things she needs to do to go home. Right now she is getting 14 different doses per day😳😳 I’m going to need some serious scheduling to keep track of all of that! She is on a med for her heart, two diuretics, vitamin d, sodium, and a reflux medicine and is getting multiple doses of each. Poor sweet baby. We had a long chat with a cardiologist last week and she was emphasizing how important it is that she is gaining weight for us to go home so I️ have been constantly asking nurses for updates on that. She goes up a little or stays steady most day but she has lost a couple of days. It doesn’t help that she is on diuretics which make her pee out all her fluids! She had an X-ray and an echo on Friday and both looked like there wasn’t much change from the previous ones which is good. Her feeds are now at 1.5 hours and we are trying to get down to one hour. She has been doing really well with it though and hasn’t been refluxing too much. Tomorrow we are going to start to wean the nasal cannula. She is just getting a fast flow right now at 2 liters so it basically just blows and helps her lungs and airway to open up. We are going to go down by half a liter each day this week if she does well. The dr has put in some of our going home orders so we have been getting a lot of the education stuff that we need to do to go home (cpr and gtube vids etc) and her gtube home pump and everything should be coming soon! Her ENT surgeon said he might be able to do her next bronch a little sooner since he is on call so I’m hoping that happens! And they decided to wait until a week from Tuesday to discuss her case at the cardiac conference- but if she is ready to go home before then we won’t need to wait for that to happen. She hit six weeks yesterday and is just about 8 lbs exactly and is in the 15th percentile for everything.
November 16th, 2017 9:43 PM
Cece had her bronch today!! This was the last big thing we were waiting for. Dr Brigger her ENT put the scope down and the scar tissue (subglottic stenosis) was growing back more than last week. It still wasn’t super bad but he couldn’t do nothing about it. He injected it in three places with steroids and did the balloon dilation. So it didn’t go perfectly because he hoped to have to do nothing, but he is still ok with us going home on Monday. She managed to not need to get intubated luckily so that was good! Since he had to actually mess with her airway she has been pretty fussy and in pain today poor baby😭 her primary nurse is with her tonight and hopefully she can get that pain under control. Brigger wants us to come back about two weeks after thanksgiving for another bronch and we will have to stay the night hopefully in the nicu again. But at least we get to go home before that!
A few days ago they started adding calories to her feeds because she was kind of plateauing with her weight. So they just add formula to the breast milk to give it more bang. She was a little gassy yesterday but otherwise seems to be doing well with it. She still hasn’t gotten much over 8 lbs but hopefully this helps to fatten her up more quickly! Also she got completely off her oxygen today! They had slowly been weaning it and took it off after her bronch and she has done awesome without it! And we got her stupid IV out of her head thank heavens. She still has her picc line in but they will take that out over the weekend and she will just have the regular monitors on!
I️ seriously can’t believe we are really bringing her home though! They ordered all of her meds, her home g tube pump is coming Monday, we are starting to make all of her follow up appointments with her many drs. I’m trying to make sure I’m totally prepared but it’s going to be a little scary still.
Also she is going to be getting synagis shots which are reserved for only super high risk babies or ones who were earlier than 29 weeks. They are shots that should help her with the flu/cold season and to not get RSV. I’m so glad she’s getting them but sad that she is in the category where she needs to get them.
Now we just need her to stay stable this weekend and gain weight and breath well and we will be home!! Monday will be 51 Days